 What is a safe anesthetic? I’d have to say that it’s one you wake up from without any apparent damage.
What is a safe anesthetic? I’d have to say that it’s one you wake up from without any apparent damage.
OH… you meant which anesthetic is safe for your pet? Well, that is a good question.
I have heard anesthetics described as poisons, and that seems a bit extreme. On the other hand, if they were good for you, you wouldn’t lose consciousness.
Of course, loss of consciousness, at least the consciousness of pain, is what we are trying to achieve with anesthesia. That’s what the word means: no pain.
 You watch the scene in “Gone With the Wind” where they are out of anesthetic and need to cut off somebody’s leg… it’s not my favorite part of the movie.
You watch the scene in “Gone With the Wind” where they are out of anesthetic and need to cut off somebody’s leg… it’s not my favorite part of the movie.
Or take a look at the mini-series “John Adams”, starring Paul Giammati. His daughter has a mastectomy while four people hold her down and she bites on a leather strap so she doesn’t bite her tongue in half.
Anesthetic may not be good for you, but most of us would prefer it to four guys holding us down while we get an amputation.
There’s a great episode in the old “John Nesbitt’s Passing Parade” short subjects depicting one of the first successful abdominal surgeries performed with anesthesia. It was a fundamental change in the treatment of disease and injury. Anesthesia is a good thing when it works.
Originally I talked about loss of consciousness. Most patients under good anesthesia do not react to painful stimuli. They don’t struggle, or have elevated heart rates, and people don’t remember anything about it. That is, most of them don’t. There are documented cases of patients who lay still all during their operation, but were able to recall every moment of it, including the operating room conversations. So that gets you into a discussion of what constitutes consciousness… which is not what we’re talking about.
We’re talking about which anesthetic is safe for your pet.
 You’ve probably heard it said that flying a big airplane is 99% boredom and 1% sheer panic. Anesthesia is like that. When it’s going well, there’s not much to do. When the patient has a problem, you have to be on top of it and get something done in a hurry.
You’ve probably heard it said that flying a big airplane is 99% boredom and 1% sheer panic. Anesthesia is like that. When it’s going well, there’s not much to do. When the patient has a problem, you have to be on top of it and get something done in a hurry.
It may be a truism, but I have to agree with the statement that there are no “safe anesthetics”, just safe anesthetists. It’s not so much about which anesthetic drug combination is the “safe” one, but how a doctor can produce a safe anesthetic experience.
Sixty years ago, most veterinarians were using intravenous sodium pentobarbital for anesthesia. You give enough to “knock the animal out”, and it lasts quite a while. You can give more if they start to wake up, but you can’t give less. It’s just in there. The animal doesn’t thermo-regulate while it’s out – body temperature falls, and so does blood pressure. Despite this, veterinarians performed many successful procedures. They learned how to use the drug safely.
Of course, the drug wasn’t very “adjustable”, and you were likely to have problems, and even lose the patient when the animal was in poor health, severely traumatized, or very old.
With the anesthetic agents we have now, we have many more options and the drugs have wider margins of safety. You can titrate the dose, giving the drug until the patient is just “deep enough” and maintain them at that level. You can back it off if they are too deep, you can increase the dose if they aren’t deep enough. In other words, these drugs are easier to use safely than our older drugs.
 Unfortunately, safer drugs alone do not make for a safe anesthetic experience. Sevoflurane gas can still be overdosed. It takes a while, but you can do it. Propofol is a great drug, but they managed to kill Michael Jackson with it.
Unfortunately, safer drugs alone do not make for a safe anesthetic experience. Sevoflurane gas can still be overdosed. It takes a while, but you can do it. Propofol is a great drug, but they managed to kill Michael Jackson with it.
Appropriate dosing is important, and this must take into account a lot of things besides just the species, size, weight and age of the patient. You need to factor in any other medical conditions, nutritional status, stress level, and so forth. There are some breed-specific problems that you have to consider.
Pre-anesthetic risk factors need to be assessed. Is there any problem with heart or lung function? Chest X-rays and electrocardiogram can tell you. What about liver or kidneys? They help rid the body of some drugs, and they are sensitive to poor circulation. Blood tests can let us know about problems we cannot see from the outside. A patient who might otherwise be fine for a short procedure may need to be on intravenous fluids for support.
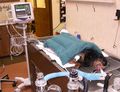
The most important thing that you do is to pay attention to how the patient is doing. When I was in veterinary school in the seventies, you learned to monitor the patient with hands-on constant observation. You looked at color and capillary refill time, you felt the pulse, you listened to the chest. This is not a bad way to do things, but now we have access to tools that can give us a lot more information without constantly poking the patient.
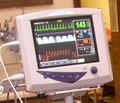 The patient is connected to this monitor and I can see at a glance the electrocardiogram, the depth and rate of each breath, the oxygen saturation, the carbon dioxide build-up and the blood pressure. The instant that something changes, we see it and hear it and can take steps to deal with it.
The patient is connected to this monitor and I can see at a glance the electrocardiogram, the depth and rate of each breath, the oxygen saturation, the carbon dioxide build-up and the blood pressure. The instant that something changes, we see it and hear it and can take steps to deal with it.
These are the things that make for a safe anesthetic experience:
- Knowing the patient’s condition
- Choosing a drug combination that should be appropriate
- Having an anesthetic regimen that can be adjusted “up or down” as needed
- Supporting the patient with warming devices, intravenous fluids, and other drugs as needed.
- Monitoring the patient’s condition so that you know when you need to “do something”
It is quite rare to lose a patient as a result of the anesthetic, but it can happen. Even with all the best equipment and the most expert anesthetist at a university teaching hospital, there is no way to guarantee a good outcome every time.
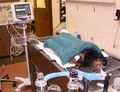 With today’s medicines and techniques, we are able to successfully perform long and complex procedures on some really old, sick animals. Nothing is 100% safe in this world, but a safe anesthetist can usually provide a safe anesthetic experience.
With today’s medicines and techniques, we are able to successfully perform long and complex procedures on some really old, sick animals. Nothing is 100% safe in this world, but a safe anesthetist can usually provide a safe anesthetic experience.

